Pavilion Publishing and Media Ltd
Blue Sky Offices Shoreham, 25 Cecil Pashley Way, Shoreham-by-Sea, West Sussex, BN43 5FF, UNITED KINGDOM
In this article, you are asked to guess the diagnosis between: pityriasis rosea, gutatte psoriasis, pityriasis lichenoides et varioliformis acuta, and secondary syphilis.
The case
James is a 22-year old music student. He comes to see you about a rash that started on both arms and hands, and which has spread to his chest and legs over the past three days. John regularly goes to the gym and is becoming very self-conscious about it. He complains that the rash is very itchy.
On examination you notice a large number of papules on both legs, arms and his chest with a slight degree of scaling on a small number of lesions.
At the moment, James is a little anxious. He has a final recital exam in a weeks’ time. He went to see his GP two days ago and was prescribed 20mg propranolol, up to three times daily to help with his performance anxiety.
James has no other medical problems or a history of skin problems (though seems to remember that his father had very scaly skin over his elbows). He mentions in passing, almost as an afterthought, that about 10 days ago he had a bad cold and lost his voice for a few days.
Based on the information provided and the images, what is the most likely diagnosis?
|
Answer: gutatte psoriasis
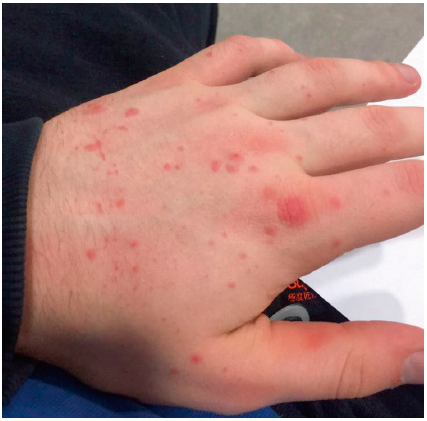
In this case the most likely diagnosis is gutatte psoriasis.
The word “guttate” comes from the Latin word gutta which means drop and the condition is characterised by numerous, small, salmon-pink, “tear drop” like, scaly lesions which affect the trunk and limbs. Lesions are approximately 1cm in diameter, though in the early stages little scale in visible. The guttate form is relatively uncommon and affects around 2% of those with psoriasis and occurs with an equal prevalence in both sexes. The rash usually develops quickly (within a couple of days) and tends to affect children and young adults.
Pityriasis rosea is thought to be a viral rash (although it is not contagious) that will often last for between 6 and 8 weeks and while it can be pruritic, it is often asymptomatic.
It is estimated to affect around 1.3% of the population, most commonly during autumn and spring. Unlike gutatte psoriasis, classically, pityriasis rosea starts with a single larger lesion (the Herald patch) which is present in 50-90% of cases. The patch initially presents as a pink papule that may be mistaken for other conditions such as insect bites. The lesion evolves and enlarges to between 2 and 10 cm in diameter with a central salmon-coloured area, and a darker red peripheral zone has a collarette of fine scale (i.e. collar-like scaling at the periphery of the lesion) just inside of the well-defined border. Typically, the Herald patch is found on the abdomen, chest, back or neck. In some patients, there are prodromal symptoms (malaise, nausea, fever, headache and joint pain) preceding the appearance of the Herald patch.
Over the next one to two weeks, crops of smaller (0.5 to 1.5 cm), elliptical or oval macules and papules with a collarette of scale develop symmetrically commonly on the trunk, but can involve the limbs and normally spares the face, hands and feet. The lesions are a dull pink colour with peripheral scale.
Pityriasis rosea is thought to be a viral rash (although it is not contagious) that will often last for between 6 and 8 weeks
Pityriasis lichenoides et varioliformis acuta is an acute outbreak of 10 to 50 small, reddish brown papules, 5 to 15 mm in diameter. It is a rarely seen condition – one study found 17 cases in 44,000 patients over a 10 year period. It can be differentiated from guttate psoriasis in that the papules become vesicular and develop haemorrhagic crusts. The condition is most commonly seen in children and young adults, with a slightly higher prevalence in males. Although the precise cause is unknown, it is suspected as being a T-cell mediated response to an environmental viral antigen and, occasionally, patients experience mild symptoms such as fever, headache and malaise prior to the development of the condition.
The development of a solidary, small, red papule that quickly ulcerates (chancre) and which can develop on the penis, inside the vagina or anus is the hallmark of an infection with syphilis. If left untreated,secondary syphilis develops in around a quarter of those with a primary infection, around 6 weeks later. It presents as a symmetrical rash and unlike gutatte psoriasis, the eruption initially presents as oval macules that rapidly develop into red-brown (coppery red) papules on the trunk that for a short time may scale. The rash frequently presents on the palms, soles and face but unlike gutatte psoriasis, are classically non-pruritic. Patients may also develop fever, swollen lymph glands, muscle aches and fatigue.
What features in the case history support your conclusion?
|
Why gutatte psoriasis?
In this case, the most likely features that support the diagnosis are James’s recent cold and sore throat, i.e. a streptococcal upper respiratory tract infection, the likelihood that his father may have had psoriasis (i.e. the presence of a family history) on his elbows, and his anxiety over a recital exam.
The association between streptococcal infections and acute gutatte psoriasis has been known for many years with studies finding a high incidence of streptococcal infections and raised serum antistreptococcal M6 protein in blood samples.1 One case controlled study indicated a strong association between guttate psoriasis and both a family history of psoriasis and stressful life events.2
The role of beta-blockers in aggravating or inducing any form of psoriasis is based largely on numerous case reports which have described a psoriasiform drug eruption. In an attempt to clarify the association between use of beta-blockers and psoriasis, one large case-controlled analysis of the UK General Practice Research database, included data on more than 36,000 cases with a first-time diagnosis of psoriasis with matched controls. The study concluded that beta-blocker use, or in fact any other antihypertensives, are not associated with an increased risk of psoriasis and there was no evidence that such drugs induced guttate psoriasis.3
What course of action would be most appropriate for this patient?
|
What to do?
In this case, the most appropriate answer would be to advise James that the rash should resolve after a few weeks without treatment. It might be helpful to use an emollient until the condition resolves, particularly if pruritis is a problem. Topical coal tar products might be of value, since these can be applied over large areas of the body without any problems.
Vitamin D analogues are also effective, but since the drug has to applied to the individual lesions, the recommended weekly amount of 100g might be quickly exceeded when a large number of lesions are present. It would also be extremely time-consuming for the patient! In fact, according to a Cochrane review on the treatment of guttate psoriasis, the authors concluded that “there is currently no firm evidence on which to base treatment of acute guttate psoriasis”.4
There is some evidence that a daily use of omega-3 fatty acids for 10 days led to significant improvements in disease severity, though the study was conducted in adults and used an infusion, rather than fish oil capsules.5
Although streptococcal infections can trigger gutatte psoriasis, one systematic review found no good evidence that anti-streptococcal treatments, such as penicillin or erythromycin, were beneficial.6
Narrow-band UVB treatment is effective for gutatte psoriasis, but would be a more appropriate course of action for those with widespread or unresponsive disease.
Patient leaflets on gutatte psoriasis can be found at https://bit.ly/2PxR43L and https://bit.ly/2w6WZET.
References
- Zhao G, Feng X, Na A et al. J Dermatol 2005; 32(2): 91-96
- Naldi L, Peli L, Parazzini F et al. J Am Acad Dermatol 2001; 44(3): 433-438
- Brauchli YB, Jick SS, Curtin F et al. Br J Dermatol 2008; 158: 299 – 307
- Chalmers R, O’ Sullivan T, Owen CM et al. Cochrane Database of systematic reviews 2000, Issue 2. CD001213
- Grimminger F, Mayser P, Papavassilis C et al. Clin Investig 1993; 71(8): 634-43
- Owen CM, Chalmers RJ, O’Sullivan T et al. Br J Dermatol 2001; 145(6): 886-90.
Rod Tucker, Pharmacist with a special interest in dermatology.


